Not knowing when you’re going to get your period or dealing with irregular menstrual bleeding can be frustrating. Plus, irregular periods can have bigger implications, such as impacting your fertility and increasing your risk for certain types of cancers.
You may be wondering how to get regular periods naturally. Indeed, some strategies can help support a more consistent menstrual cycle.
Around 14 percent of people who bleed have irregular periods according to research published in the journal American Family Physician. If this sounds like you, you may just need to audit some lifestyle factors—like diet, sleep, and stress—that could be contributing to hormonal imbalances.
Here's how you support your cycle and potentially reduce some unpredictability.
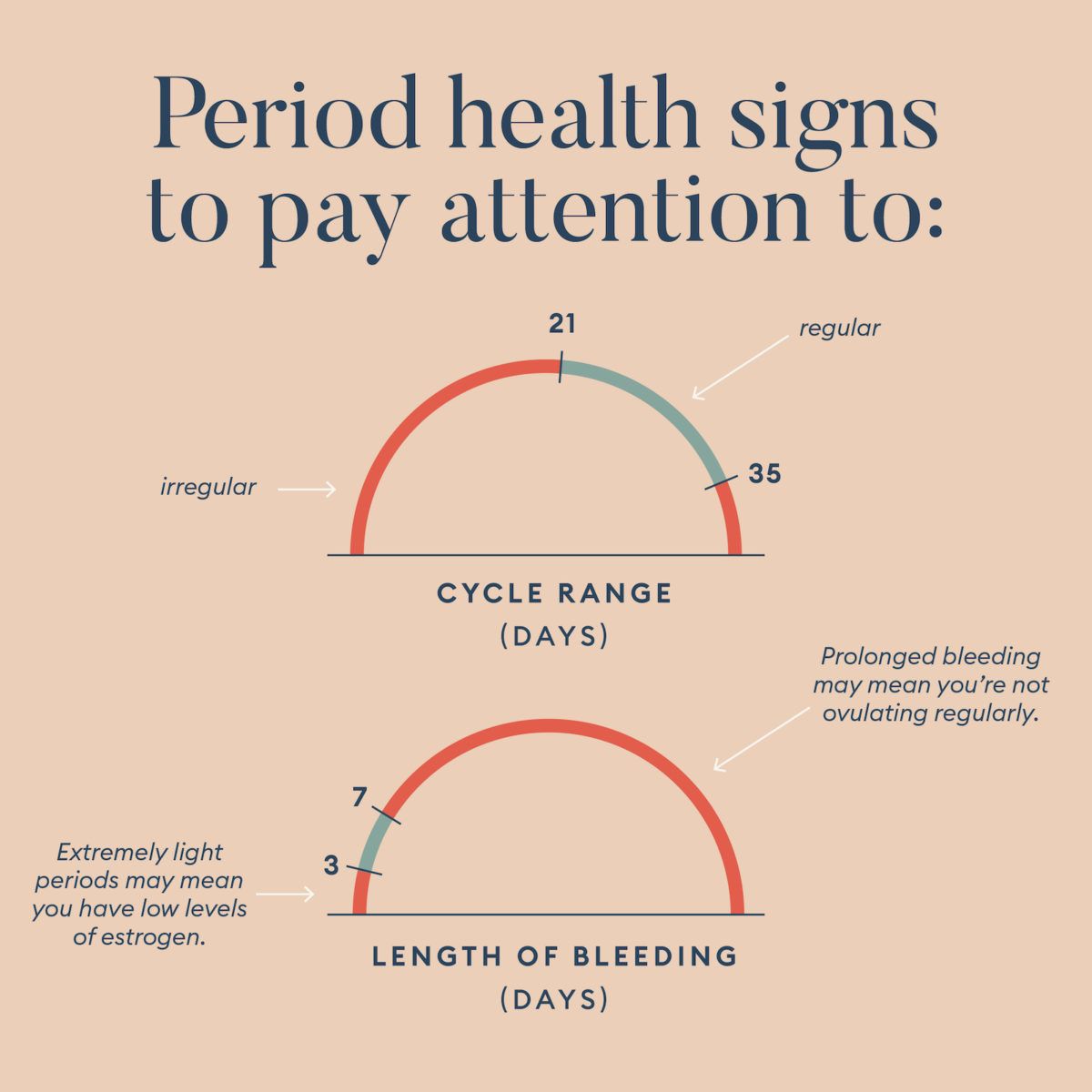
What is an irregular period?
Normal cycles can be anywhere between 21 and 35 days, says Tiffany Lester, MD. But if you’re finding that your cycle is repeatedly falling into a pattern of much shorter or longer than this range, you may have a hormonal imbalance.
PMS symptoms like cramps, bloating, and mood swings are common in the days or even a week leading up to your period, and these symptoms can signal that you're about to menstruate.
“Depending on how in tune with your body you are, you may also be able to sense when you’re ovulating,” Dr. Lester says. If ovulation doesn’t seem to sync up within about 2 weeks of your period, it could be a sign that your cycle is irregular. However, 3 to 8 percent of the cycles can be anovulatory and still be normal.
Another sign of irregularity is the consistency of the blood you’re seeing, Dr. Lester points out. You may experience spotting beforehand or throughout your cycle and then not see bright red blood on the first day of menstruation.
“That could be a signal that you may have a hormonal imbalance like low progesterone,” she explains. Keep in mind that you can still have a regular 28-day cycle but have inadequate sex hormone levels, says Dr. Lester.
If you think your period falls outside a normal pattern, ask your doctor about it, as it could be a sign of a deeper issue.
Here are a few reasons your period could be off.
Causes of irregular periods
1. Stress
Stress doesn’t just affect your mood. It can have all kinds of effects on your body, including skipping a period here and there. “We all respond to stress differently, and it can cause you to miss a whole month altogether,” Dr. Lester says.
The stress hormone cortisol is intricately connected to the hormones estrogen and progesterone, and has the ability to throw off your cycle completely.
“If cortisol is high, it can deplete progesterone, which you need to completely finish the second part of your cycle to build up the uterine lining and prepare for either pregnancy or shedding the lining and having your period,” explains Dr. Lester.
2. Lack of sleep
Not getting enough sleep or having an irregular sleep pattern can also cause irregular periods. That’s because your circadian rhythms are linked to your menstrual cycle. This is one reason why shift workers may experience irregular periods. Dr. Lester adds that the quality of your sleep matters too.
3. Travel
Are you constantly jet-setting, especially across different time zones? Travel can alter your sleep patterns and your stress levels and therefore your period.
But if you find that your period is irregular for more than two cycles, you should bring that concern to your doctor, Dr. Lester says.
4. Bouts of unhealthy eating and drinking
Excessive consumption of alcohol, refined carbohydrates, and sugar can affect your hormones. Even one glass of wine can increase your estrogen levels, Dr. Lester explains.
The inflammation associated with excessive drinking or overeating carbs and sugar can mess with the sex hormones that regulate your cycle, she adds.
“On top of that, add in the preservatives and chemicals found in processed food and it’s a perfect storm,” says Dr. Lester. This increased inflammation can lead to irregularity or additional cramping and bloating.
5. Hormonal imbalances
One key reason for irregular periods might be a pre-existing hormonal imbalance. Some women who have estrogen dominance may experience irregularity, says Dr. Lester. But an imbalance with progesterone may also lead to an irregular period.
Polycystic ovary syndrome, or PCOS, is one of the most common hormonal imbalances that cause irregular periods. With PCOS, the ovaries make too much testosterone, which inhibits ovulation. When ovulation is irregular, the whole cycle can get thrown off.
“Parsley Health offers specialty testing for hormonal imbalances, particularly caused by thyroid issues or digestive dysfunction,” Dr. Lester says. The team will test your levels of progesterone, estrogen, and testosterone.
6. Getting off birth control
“Typically, birth control regulates your cycle,” Dr. Lester says. But if you’ve recently stopped hormonal contraceptives, you may notice that your cycle becomes irregular.
The first three to six months after stopping birth control are really an adjustment period for your cycle.
“Depending on how long you’ve been on it, it can take up to a year for your cycle to regulate after you get off hormonal birth control or a copper IUD,” Dr. Lester explains.
7. Genetics
Genetics can also play a role in how we metabolize hormones, especially when changes to diet, stress, and sleep also occur.
How do irregular periods affect your fertility?
The main reason irregular periods can make fertility tricky is because they make tracking your cycle and knowing when you’re most fertile more difficult.
You have six peak fertility days in a month, Dr. Lester points out. So if you have a hormonal imbalance, getting pregnant could become even more challenging.
“If periods are irregular because you’re deficient in progesterone, your uterine lining likely can’t support implantation, even if you’re ovulating,” she says. If you have PCOS, you may not be ovulating at all or ovulating irregularly.
To get a better handle on tracking your fertility when you have irregular periods, Dr. Lester recommends ovulation strips, which show you when you’re ovulating, or trackers that measure your basal body temperature, which is your temperature at rest.
Your basal body temperature tends to drop before ovulation and rise afterward, so it can provide insight into where you are in your cycle.
Other indicators of ovulation are the consistency of your cervical mucus. It’ll be thicker and whiter during peak fertility. And you may notice an uptick in your sex drive as well.
How to regulate your period naturally in 4 simple steps
No miracle trick will make menstruation happen on time, and what’s “normal” for you may be different than what’s normal for others.
However, here are a few hacks that can help regulate your cycle as much as possible.
1. Get into a regular sleep, exercise, and stress management routine.
We’ve already established how important regulating your sleep is for keeping your circadian rhythms on track, but maintaining consistency with your workouts is just as important.
“Exercise helps to eliminate toxins via sweat and the lymphatic system, balances blood sugar, and reduces cortisol, at which high chronic levels can deplete progesterone,” explains Dr. Lester.
One study found that anxiety and other manifestations of stress are likely to reach their peak during the pre-menstrual period.
Getting your workouts in, and maybe even incorporating mind-body movement like yoga, helps support your mental health.
2. Incorporate cruciferous veggies into your meals.
“Certain foods, like cruciferous veggies (kale, broccoli, and many dark, leafy greens) contain a component called DIM, which helps eliminate estrogen and balance hormones,” Dr. Lester says.
Studies have shown that the DIM found in these veggies can help metabolize estrogen and decrease the risk of estrogen-sensitive cancers.
3. Make sure your diet includes fermented foods.
Fermented foods like kimchi and tempeh help increase the number of good gut bacteria in your system. “That will help balance the estrobolome, the group of enzymes that help metabolize estrogen in the intestine,” Dr. Lester says. And that proper balance of estrogen can help regulate your cycle.
4. Load up on fiber.
An overall healthy diet is important for supporting your menstrual cycle, but there’s one key macronutrient in particular that can help you stay regular in more ways than one: fiber.
Research has shown that food with enough fiber in it (such as cruciferous vegetables, berries, and whole grains) help to speed up the metabolism of estrogen in your gut.
Dr. Lester suggests adding 1 tablespoon of freshly ground flaxseeds to your morning smoothie for a solid hit of fiber every day.


