This article has been medically reviewed by Nisha Chellam, MD. It contains additional reporting by Angela Myers.
What do Hashimoto’s disease, Lupus, and Rheumatoid arthritis have in common? They are all autoimmune diseases that can be reversed or slowed down when caught early. Autoimmune conditions impact between 24 and 50 million people in the United States—and millions of cases are currently undetected. These conditions are frequently missed by doctors because the early warning signs of autoimmune disease can be hard to detect.
Hard, but not impossible. Below are five early warnings to watch out for. If experiencing any, it's best to consult a healthcare provider to determine the underlying cause and a treatment plan.
What is autoimmune disease?
Autoimmune disease occurs when your body is unable to tell the difference between your own cells and foreign cells, making you more susceptible to infections and causing inflammation that leads to redness, pain, and swelling. Normally, your body’s immune system attacks germs like bacteria and viruses, but with an autoimmune disease, proteins called autoantibodies attack healthy cells.
Some common autoimmune disease symptoms include unexplained rashes, body aches, brain fog, and more—and can be more or less severe depending on the type of disease.
Types of autoimmune disease
There are over 80 types of autoimmune diseases, such as Type 1 diabetes and multiple sclerosis, that attack different parts of your body. Some of the most common types of autoimmune diseases are:
Rheumatoid arthritis
Lupus
Celiac disease
Hashimoto’s disease
Sjögren’s syndrome
Polymyalgia rheumatica
Multiple sclerosis
Ankylosing spondylitis
Type 1 diabetes
Alopecia areata
Vasculitis
Temporal arteritis
What causes autoimmune disease?
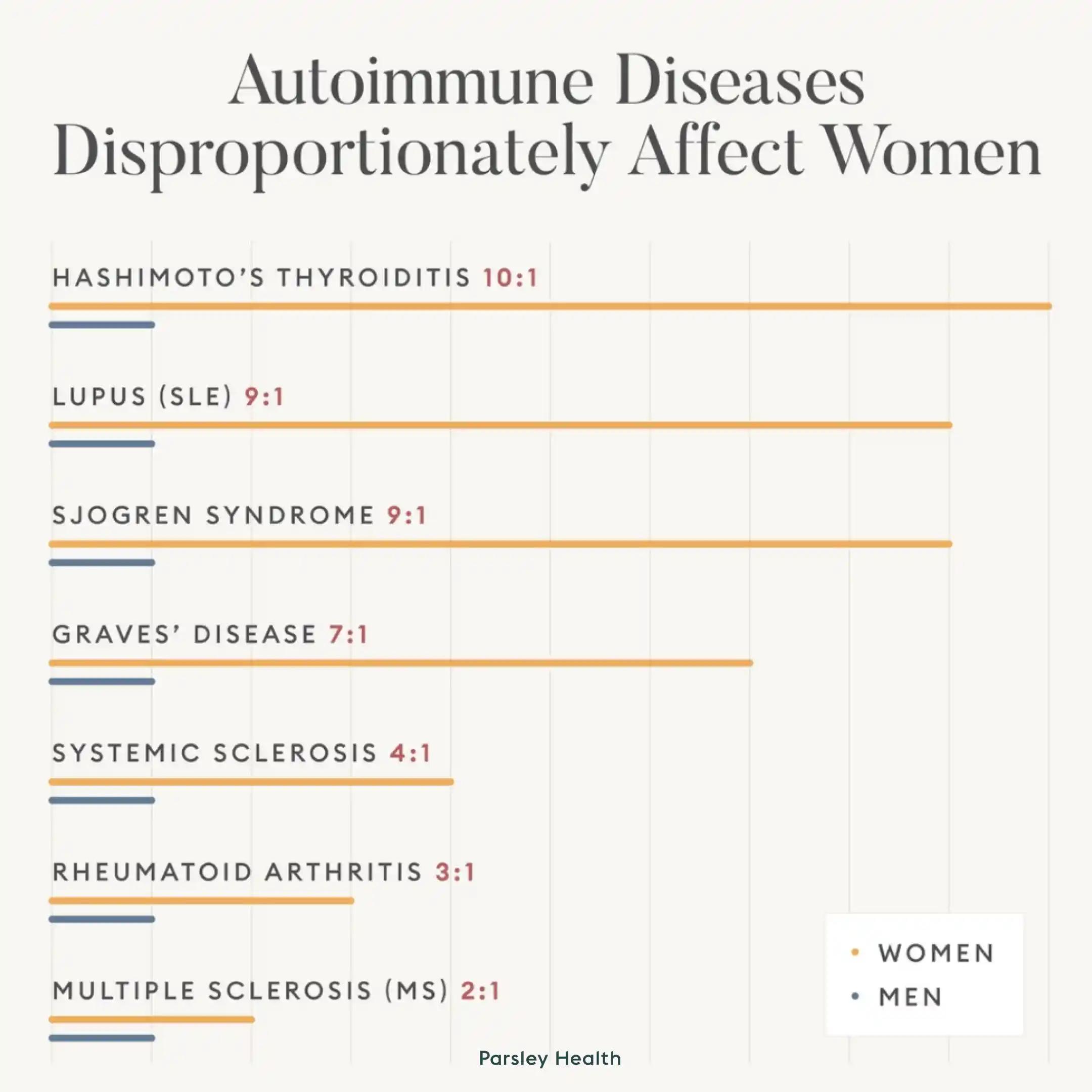
Doctors and researchers are still unsure of what causes the confusion in your immune system that leads to autoimmune disorders, though recent research has led some scientists to think the western diet or environmental factors may play a role. However, there are certain populations that are more susceptible to developing them. For example, women are twice as likely as men to develop an autoimmune disorder. Different ethnicities are also more likely to develop certain autoimmune diseases and some diseases, like lupus and multiple sclerosis, have a genetic component.
Here are 5 early warning signs of autoimmune disease:
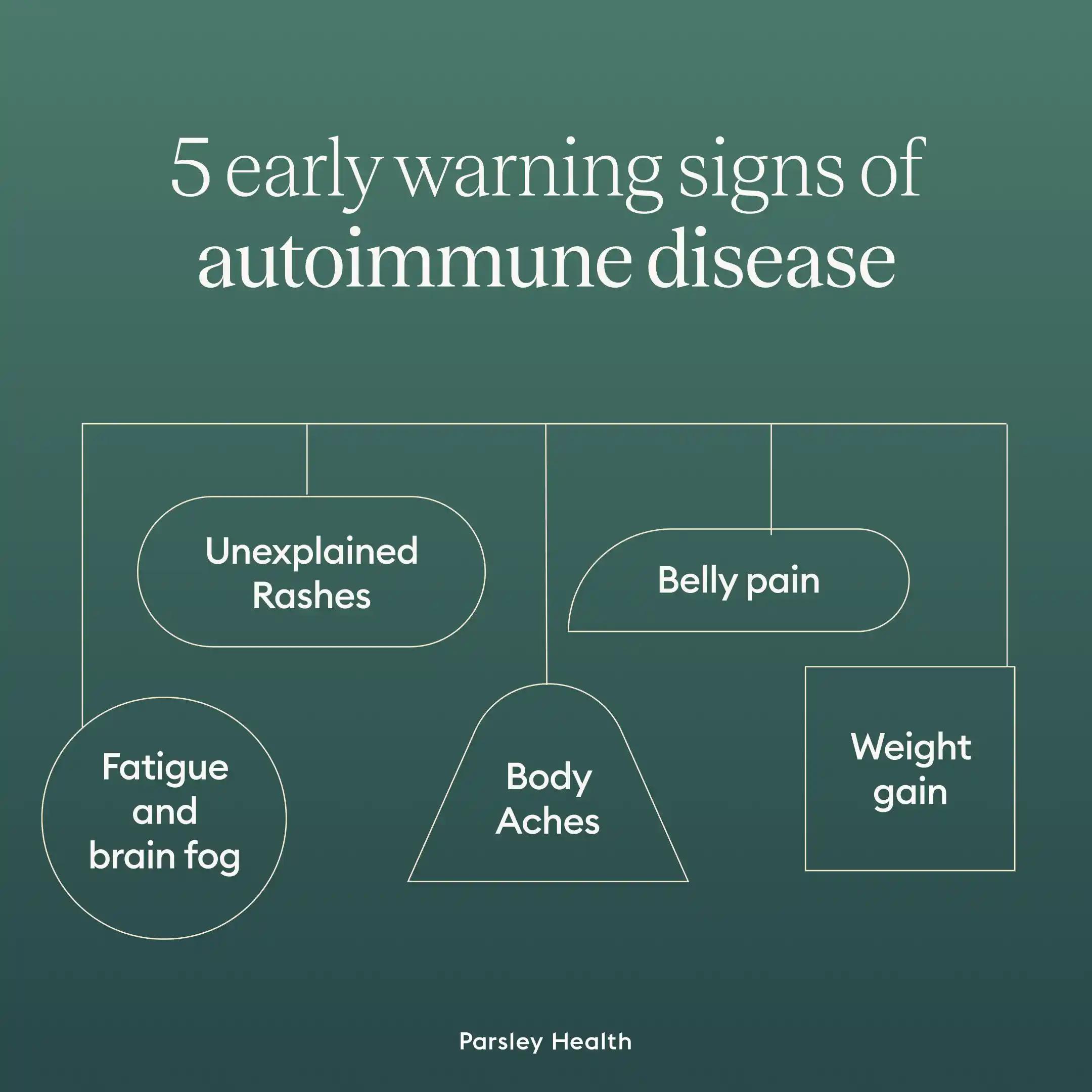
1. Unexplained rashes.
Your skin is a great mirror for the level of inflammation in your body. Red, itchy, blotchy or scaly rashes that come and go can be an early warning sign of autoimmune diseases like lupus or psoriasis. Even acne and eczema can be signs that there is underlying hyperactivity of your immune system—food sensitivities like sugar, gluten and dairy are frequent triggers, but autoimmune disease shouldn’t be ruled out.
2. Body aches.
Unexplained persistent muscle pain and joint pain can be a sign of Hashimoto’s disease, Lupus or Rheumatoid arthritis. If you hurt all over and it’s not from your workout, you may need blood work and even x-rays to rule out an autoimmune disorder.
3. Fatigue and brain fog
If you feel foggy and exhausted despite getting at least 8 hours of quality sleep, you could have underlying immune dysfunction. Sometimes fatigue is a sign of anemia or chronic disease, a type of low blood count that develops when there is underlying inflammation in the body. This can be one of the earliest signs of an autoimmune deficiency.
4. Belly pain
Sometimes people think that diarrhea cramping and bloating that come and go are just the hard knocks from eating one too many take-out meals, but if you frequently have abdominal discomfort, autoimmune diseases like Crohn’s and Celiac could be the issue. It’s much better to catch these conditions early as the longer they persist the more damage they can do to the digestive tract.
5. Weight gain
If you feel like your metabolism has stalled, maybe it has, and it might not be that glass of wine—it might be a thyroid condition. Hypothyroidism affects as many as 1 in 8 women in their lifetimes. It can be caused by nutrient deficiencies, chronic stress, inflammation, and waxing and waning autoimmune activity.
Most doctors don’t routinely test for thyroid antibodies but at Parsley they are part of our proprietary baseline panel that we order for every member. If caught early and addressed with functional medicine sometimes these antibodies will go away entirely, or at least stabilize and not cause further thyroid destruction.
6. Hair loss
Have you noticed your hair thinning or bald patches forming on your head? Brittle hair and hair loss are one of the many autoimmune disease symptoms linked to Graves’ disease and Alopecia areata. In the case of Graves’, fine brittle hair is accompanied with insomnia, irritability, weight loss, shaky hands, and more, while Alopecia areata is an autoimmune deficiency that strictly impacts the health of your hair follicles. The immune system attacks the follicles, preventing hair growth, resulting in patchy hair loss.
Preventing autoimmune disease
Autoimmune diseases are, in part, caused by genetics, meaning they are not 100% preventable. That being said, certain actions reduce your chances of either being diagnosed or may help slow an autoimmune disease.
These actions also contribute to a healthy lifestyle: eat an anti-inflammatory diet, exercise regularly, manage stress, and get enough sleep. Some studies suggest getting enough Vitamin D, either from sunlight, supplements, or food, may reduce the risk of getting an autoimmune condition too.
When to seek medical help
If experiencing any symptoms, it's best to make an appointment with a doctor to discuss potential causes and treatment options. Typically, a doctor will order a few tests to diagnose an autoimmune condition.
Autoimmune disease tests
There isn’t one test in isolation that enables a doctor to diagnose an autoimmune disease, but rather a combination of testing, along with a comprehensive medical history and physical exam.
The process of diagnosing an autoimmune disease, such as rheumatoid arthritis or celiac disease starts with a blood test. Your doctor is looking for inflammatory markers in your blood, known as an erythroctyte sedimentation rate (ESR). This measures inflammation by means of how quickly red blood cells settle in the blood. The quicker they settle, the greater the inflammation. They’ll also look for blood count abnormalities, including anemia, which signals a deficiency in healthy red blood cells or leukopenia, a deficiency in white blood cells.
As an example, if you’re concerned Hasimoto’s hypothyroidism, a common example of autoimmune disease brought on by an underactive thyroid, your doctor will look at a complete thyroid panel. The panel includes thyroid hormone levels, thyroid stimulating hormone, as well as thyroid antibodies in your blood. Your doctor will also look for an immune response through checking autoimmune serologies that could be consistent with a number of other autoimmune diseases.
At Parsley Health, to diagnose celiac disease, we will look for antibodies in the blood produced towards gluten, known as gliadin and transglutaminase antibodies, which are suggestive of celiac disease. If these antibodies are positive, the next step would involve seeing a GI doctor who would likely perform an endoscopy and biopsies of the small intestinal tissue to rule out celiac disease. There are findings on endoscopy that are consistent with celiac disease, and this is the gold standard for diagnosis.
At Parsley Health, we also conduct microbiome testing since gut dysbiosis, or imbalances in the good and bad bacteria in your gut, often exist in those with an autoimmune disease. If a microbiome disruption is found, our first line of intervention would be to treat the gut through diet, supplements, and other lifestyle interventions.
In addition to the testing detailed above, we also look at liver function, kidney function, heavy metal toxicities, and vitamin and mineral levels for further information. Since 25 percent of patients with an autoimmune disease are likely to develop an additional type of autoimmune disease in the future, we make sure to cover all the bases with our high-tech in depth diagnostic testing.
What to ask your doctor
Do my symptoms sound like an autoimmune condition?
What tests do you recommend ordering and what will they test for?
What is my diagnosis?
Are there any lifestyle changes you recommend making?
How can I best manage symptom flare-ups?
Living with autoimmune diseases
Currently there is no cure for an autoimmune deficiency, but with diet and lifestyle changes and in some cases, medication, most people are able to manage their symptoms.
Treatment plans for autoimmune disease will really vary based on the condition. Many can be managed with nutrition and lifestyle changes, supplements, and sometimes medication.
In the case of Celiac disease, many patients will go into complete remission after removing gluten from their diet, while other autoimmune diseases involve a more complicated, individualized approach. One dietary approach we find helps for many of our members with an autoimmune disorder is the AIP diet.
The Autoimmune Paleo Diet
The Autoimmune Paleo Diet (AIP) is a great way to manage autoimmune symptoms. It works by healing your immune system and gut lining through nutrition and lifestyle changes. This variation of the Paleo diet relies on 30 days of elimination of foods like dairy, gluten, grains, legumes and more, and slowly re-introducing them to help you uncover which foods produce a reaction. The goal is to relieve your symptoms, heal your gut microbiome, and decrease inflammation.
However, the AIP diet is restrictive and should be undertaken with supervision from a medical professional. Other anti-inflammatory diets that are less restrictive, such as the Mediterranean diet, may also be beneficial to people with autoimmune conditions.
A good diet can reduce autoimmune condition symptoms (not prevent) and should be accompanied by quality sleep, physical activity and stress management techniques.
Self Care Tips
Self care should be part of anyone's daily routine, but it's especially important for individuals with autoimmune conditions. The CDC provides some self care tips specific to lupus and other autoimmune diseases:
Have a system to remember to take prescribed medications
Communicate any concerns with your doctor
Rest when needed to conserve energy levels
Find a way to move your body (that you enjoy)
Eat a healthy diet
Time for activities you enjoy
Remember, every individual is different. What works for one person may not work for another, making it crucial to consult a healthcare provider before making changes to your diet, lifestyle, or treatment plan.
Frequently Asked Questions
How do autoimmune diseases make you feel?
Autoimmune disease symptoms can vary, but many people report feeling fatigued or tired more often than usual. Other common symptoms include unexplained brain fog, body aches, and weight gain.
How do you know if you have an autoimmune disease?
Autoimmune conditions are tricky to diagnose because symptoms come and go. Five early signs to look out for include:
What are the 3 most common autoimmune diseases?
While there are over 80 autoimmune conditions, three of the most well-known are Rheumatoid arthritis, Hashimoto's disease, and Lupus. Other common autoimmune diseases include Crohn's disease, Graves' disease, Type I Diabetes, Celiac disease, and Multiple Sclerosis.
How long can a person live with an autoimmune disease?
Autoimmune diseases aren't usually fatal. Most people with autoimmune conditions have a typical life expectancy. With a proper treatment and management plan, you can live a long, healthy life.
Do autoimmune diseases go away?
Autoimmune diseases are lifelong conditions and, in general, cannot be cured. That doesn't mean someone with an autoimmune condition will live with unmanageable symptoms. A proper treatment plan can reduce the amount of symptom flare-ups significantly.
Key Takeaways
Symptoms of autoimmune diseases are not to be taken lightly. Visit a healthcare provider if you're experiencing any of the following: unexplained rashes, body aches, fatigue, brain fog, belly pain, or weight gain.
Once diagnosed with an autoimmune disorder, your body becomes more susceptible to developing an additional autoimmune disorder, so make sure your primary care provider is covering all the bases when running tests.
Don’t let an autoimmune disease stop you from living your life. While it might be frustrating to find what works best for you at first, we’ve seen patients live healthy, fulfilling lives, and in many cases reverse their conditions.


