You may not be able to see it happening, but inflammation is the body’s interior defense mechanism toward anything going wrong, like illness or injury—it occurs with anything from a bruised elbow to an aggravated gut barrier. The catch? Inflammation can be both good and bad.
There’s no shortage of news these days about inflammation, the buzzy word that sounds at once protective and destructive. Research has shown associations between inflammation and heart disease, cancer, chronic fatigue syndrome, and more. You may even have symptoms like breakouts, joint pain, or digestive issues without being aware that inflammation is really at the root of it. Not all inflammation will have a major effect on your health, and not all inflammation is permanent, either.
What is inflammation, anyway?
In general, inflammation behaves like an immune response in the sense that foreign particles, like a bacterial infection, for example, are trying to enter your system, and your body is using inflammation to fight it off—the area becomes inflamed so that nothing else can enter and do further harm. During an inflammatory response, your body boosts production of white blood cells, cytokines that fight infection, and immune cells, like neutrophils.
The main source causing the inflammation could be an allergy, infectious bacteria, food intolerance, or autoimmune disorder. Here’s how you can understand what the source of your inflammation is (or know if you have it in the first place), and how to tame it.
Chronic inflammation vs. acute inflammation
“Acute inflammation is always something that happens to your body immediately, like an infection or injury,” explains Ruvini Wijetilaka, M.D., a physician at Parsley Health New York.
Acute inflammation almost exists like padding for your bones and joints when you have an injury—it may manifest itself as swelling around your knee cap, for example, but typically goes down within a couple of days, according to research, as the injury heals.
Chronic inflammation has likely been going on for a long time before you realize it’s happening. It’s almost always associated with other conditions, Dr. Wijetilaka says, like autoimmune diseases such as Rheumatoid Arthritis. This type of inflammation could exist in a number of places throughout the body—like the nasal passages, in those who have chronic sinus issues. “The skin and gut, two of the largest organs in the body, are very common points of entry for inflammation,” says Dr. Wijetilaka.
What causes inflammation?
It’s a bit of a “chicken-or-egg” type situation with chronic inflammation because it’s so closely associated with other medical conditions. “When people have autoimmune diseases, they also have highly inflammatory states, but in someone who has chronic inflammation, to begin with [which is usually already a sign of an autoimmune condition or something similar], that may contribute to other conditions,” says Dr. Wijetilaka.
Any autoimmune disorder, where the body is building up antibodies against itself in certain areas, is likely closely related to chronic inflammation. This includes conditions such as Rheumatoid Arthritis in the joints, which causes erosion in between the bones, Hashimoto’s disease in the thyroid, Eczema and Psoriasis in the skin, Asthma and Sinusitis in the sinuses, and leaky gut and Crohn’s, an Inflammatory Bowel Disease in the gut.
If it goes untreated, chronic inflammation can lead to a host of other issues, especially in the heart and brain, Dr. Wijetilaka explains. “For the heart, long-standing inflammation is linked with heart disease. In the brain, it can contribute to Alzheimer’s disease (it was thought that inflammatory cells couldn’t cross the blood-brain barrier, but they can, it turns out), but the exact pathogenesis is not clear,” she says.
How do you know if you have chronic inflammation?
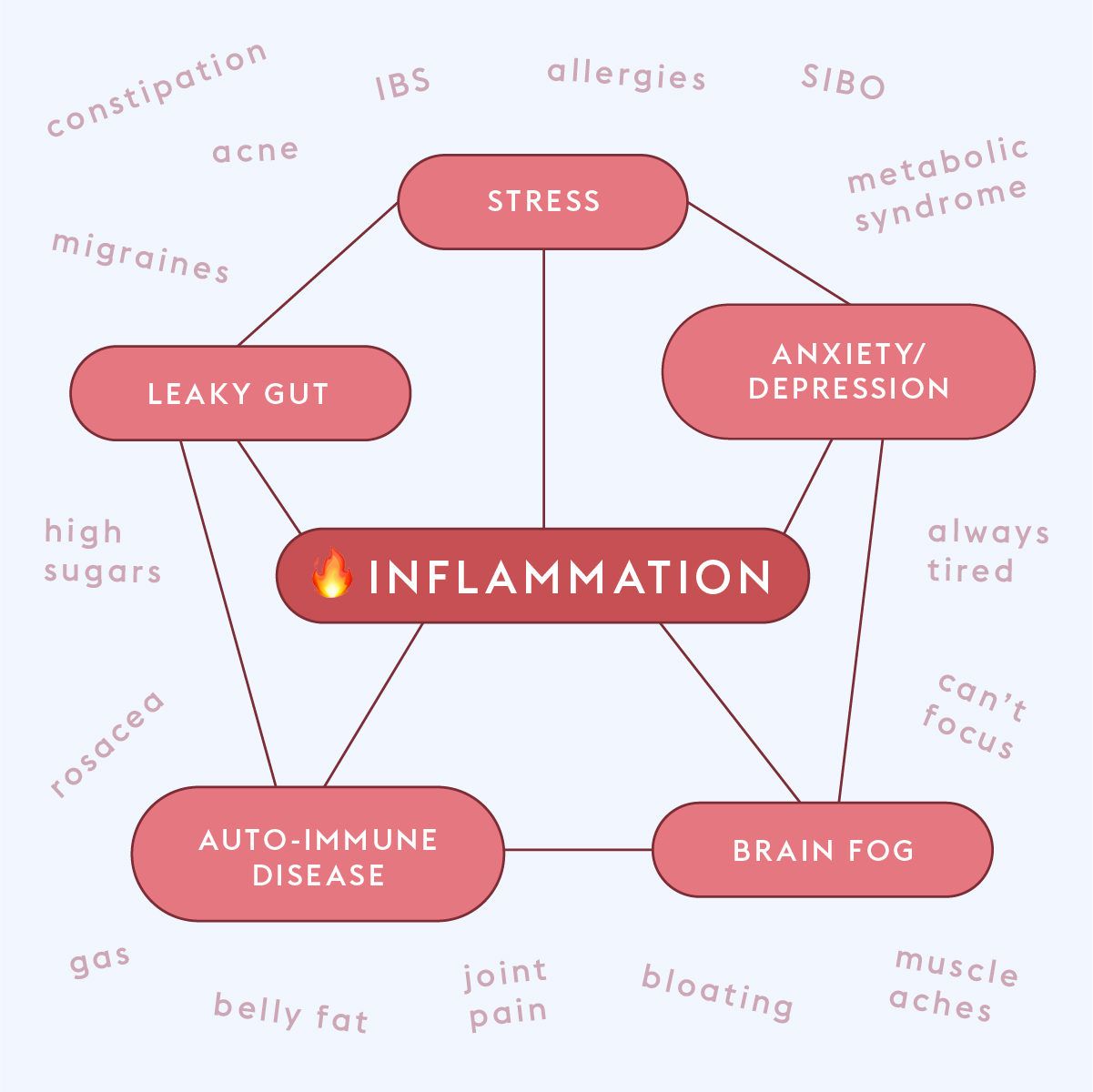
Common signals that inflammation is happening typically exist in the GI tract, the skin, and the joints. You may experience any form of GI discomfort, like diarrhea or constipation, (you may also have an associated inflammatory bowel condition). Skin symptoms usually include breakouts, hives, or rashes that appear out of nowhere, because your body is having an immune response to something. Joint pain is also common because the areas around the joints become inflamed as a mode of protection from an inflammatory agent.
Mental health symptoms are also not uncommon, Dr. Wijetilaka says. “Brain fog is a major signal of inflammation,” she says, “which includes lack of focus, not being able to think properly, and lack of mental clarity.”
There are blood tests that measure markers of inflammation, and at Parsley Health, these tests are part of the blood work each member receives. Your doctor will test for levels of two key inflammatory markers: ESR, a blood sedimentation marker, and CRP, or C-Reactive Protein, a protein made by the liver in response to inflammation. “When these levels are elevated, this tells us that there’s an inflammatory process going on,” Dr. Wijetilaka says. It’s common for practitioners to repeat this testing about every six months; if you have an autoimmune condition, it’s ideal to treat the inflammation directly so that these markers go down, closer to normal, explains Dr. Wijetilaka.
The connection between inflammation and mental health
One big driver of inflammation is stress. Stress is an enormous trigger of chronic inflammation—and it also gets worse with inflammation, which is why stress management is such a key piece of taming inflammation. Depressive symptoms may also appear. This is because serotonin, one of the body’s neurotransmitters regulating things like mood and sleep, is mostly produced in the gut. Recent research estimates that 90 percent of serotonin is released from the gut, and only the remaining 10 percent is released in the brain, so the link between gut health and mental health is stronger than we even thought. “Serotonin won’t be released properly when a person has inflammation and poor gut health, so this may cause not necessarily a clinical diagnosis of depression, but depressive symptoms,” says Dr. Wijetilaka.
How to reduce inflammation naturally
Remove foods that cause inflammation
Healing the gut is usually the first step to treating inflammation, says Dr. Wijetilaka. Eliminating dairy and gluten, inflammatory triggers for many people, can help. Processed food also aggravates gut inflammation further, especially for patients who have IBS, Crohn’s, or Ulcerative Colitis.
Stick to whole foods that reduce inflammation, like green, leafy vegetables, berries like strawberries, blueberries, and blackberries, and Omega-3-packed healthy fats like nuts and chia seeds, salmon, and tuna.
Research anti-inflammatory supplements
There are a number of supplements that you can try that may soothe inflammation. One common choice is L-Glutamine, which according to Dr. Wijetilaka, can help heal the gut lining, and decrease inflammation in the gut. Probiotics are also good for this purpose—they can restore good bacteria in the gut microbiome as well. Taking Ashwagandha or Rhodiola may help tame stress, and in turn reduce inflammation, especially in the gut. Vitamin D can also improve your mood (which makes sense because being in the sun typically does the same) booster and prevent inflammation. Another important nutrient to reducing inflammation is Omega-3’s—Dr. Wijetilaka recommends taking a supplement, because it’s difficult to get enough Omega-3’s from fish and other foods in your diet.
Practice stress-relieving techniques and activities
Any mind-body practices, for instance, yoga and meditation, can help with stress reduction, which is key to reducing inflammation and may help with those associated brain fog symptoms, Dr. Wijetilaka says. It can be as simple as using a mindfulness app on your phone to check in with yourself at the beginning or end of the day. In fact, studies have found that mindfulness practices lead to increases in gray matter in the brain, which is important for healthy cognitive function and memory retention.
Try an infrared sauna
Dr. Wiketilaka suggests giving infrared saunas a shot, in order to release toxins from the body, and reduce inflammation as well. “It helps with your joints, increasing mobility,” she adds. There hasn’t been a large amount of research on this topic, but one study suggests that far infrared therapy may alleviate some of the pain and fatigue associated with many autoimmune disorders.






